Stories from the frontline: Community nursing to COVID Intensive Care Unit (ICU) - Lia’s Story

During this continued time of uncertainty, extraordinary people are making extraordinary things happen. Nationwide, nurses, doctors, carers, and other healthcare and key workers have re-trained, been re-deployed and some have even come out of retirement to join the effort to help tackle the ongoing pandemic.
As restrictions ease, and the transmission of COVID-19 in the community decreases, people who have been redeployed within Solent NHS Trust and to other Trusts are starting to return to their normal roles. There are so many stories of people going above and beyond, with such flexibility to, help people in our communities.
Lia Wadsworth is a community practice nurse working at Solent GP Surgery. Her role involves carrying out clinics, blood tests, baby immunisations, as well as giving health promotion advice. Lia specialises in Chronic Disease management, helping people to manage their diabetes. At the start of the COVID-19 outbreak, Lia volunteered her knowledge and skills to help on the Intensive Care COVID-19 Unit at University Hospital Southampton NHS Foundation Trust (UHS).
Nurses working in the community, and particularly in the primary care setting, support people with a wide range of health needs, many of whom have more than one chronic condition. The ability to understand how this affects people and having insight into how people live in their communities is invaluable when transferring into a different care environment. The nurse will be able to use their skills and knowledge while caring for people in the hospital setting and will be able to help in planning a safe discharge home with the right support for the person and their family or carers.
“It was around March time that I started to notice that things were ramping up with the pandemic and I’d heard that some people were being re-deployed to other services. About three and a half years ago, I worked in intensive care and I’ve kept in touch with the nurses that are still working there. We had an informal conversation and they told me that they were going to need some help people who had previous experience of intensive care and trauma.
“I felt it was my duty to help, so I spoke to my manager who was extremely supportive. She said that I could go back to the ICU full-time, on a secondment basis.”
Lia was re-deployed to UHS in April, when the virus was making its way towards its peak.
“At the beginning, I didn’t really know what to expect. I thought it was going to be bedlam, but the management teams were brilliant in organising it all.
“The hospital Trust ran training on critical care assessments, donning and doffing (putting on and removing) personal protective equipment (PPE) and we were fit tested for facemasks. We were also told how to ‘prone’ a patient, which is when you transfer a patient onto their front when they are struggling to breathe – something I’d not experienced before.
“We worked on a cohort basis - this means one ICU nurse looking after five patients and we were categorised on experience. I was a category ‘A’ as I’d worked in ICU, category ‘B’ was a registered nurse who had no experience of critical care but had been brought in to help. It was a really different way of working.
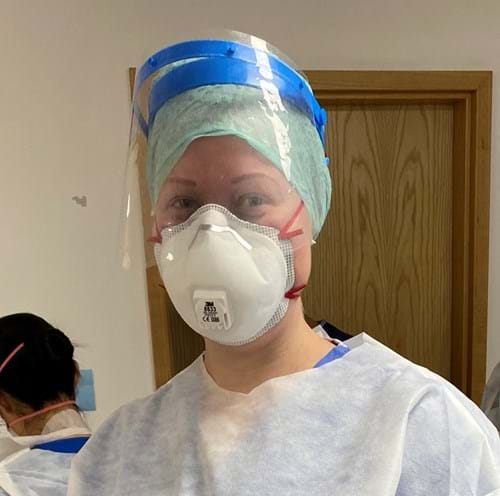
“It was really tough but the most challenging thing for me wasn’t treating a deadly disease we’d never seen before, but the PPE. We’d work in a full gown, visor, hat to cover our heads, a surgical FFP3 mask, gloves and aprons on top. The gown was like a skin, and we’d need to protect it like it was our own, so we replaced aprons for every new patient and got used to the marks made by our visors and masks.
“Coronavirus doesn’t discriminate, it’s continued to affect people of all ages from all walks of life. I’d cared for a fair few patients, but one day found myself looking after a fellow nurse, who had deteriorated rapidly and found herself in ICU. I didn’t know her personally, but that didn’t stop the situation filling me with emotion, she was one of us. I was with her when she was awake, she’d had been extubated (breathing tube removed from her trachea) and a light of hope had broken through. The sheer determination she showed throughout her recovery was amazing and I felt privileged to be part of that journey. I believe she is now recovering at home, ready to get back into the hospital caring for those in need.
“After a few years out of the critical care scene, I was happy to know my skills hadn’t gone away. Putting my experience aside, I was in awe of the other nurses who I worked alongside, who were committed to help in any way that they could. One nurse was a children’s nurse and hadn’t ever worked with adults before, but she had enthusiasm that was exceptional.
“It’s been an emotional rollercoaster. Everyone knows that some nurses can develop a dark sense of humour just to get through the day – one minute your laughing, the next minute you want to break down in tears, your sweating, your tired, but it’s an experience I’ll never forget.”